Your Provider Data Foundation for Compliance, Accuracy, and Member Trust

Health plans face relentless pressure to maintain accurate provider data amid intensifying regulatory scrutiny and compliance demands, where every error carries higher financial and reputational risk. Meanwhile, members demand seamless access to care, making data accuracy a make-or-break factor for satisfaction, retention, and competitive advantage.
Over the past two years, H1 has successfully acquired Veda + Ribbon. We’ve deliberately combined complementary strengths to solve health plan problems. Whether you’re a long-time H1 customer or come to us through Veda or Ribbon, we wanted to share how we are building a stronger data platform together.
- End‑to‑end automation. Veda’s roster automation, deep health plan expertise, and advanced scoring models are now embedded into H1, reducing manual work and elevating data quality at scale.
- Advanced connectivity. Ribbon’s APIs bring richer relationships and care context, enabling plans to move beyond static directories to true network intelligence that supports smarter access and referral decisions.
- Robust accuracy scoring. The integration of H1’s data pipeline with Veda and Ribbon improves accuracy by consolidating scoring logic and validation, elevating more provider records into top confidence tiers under CMS regulations.
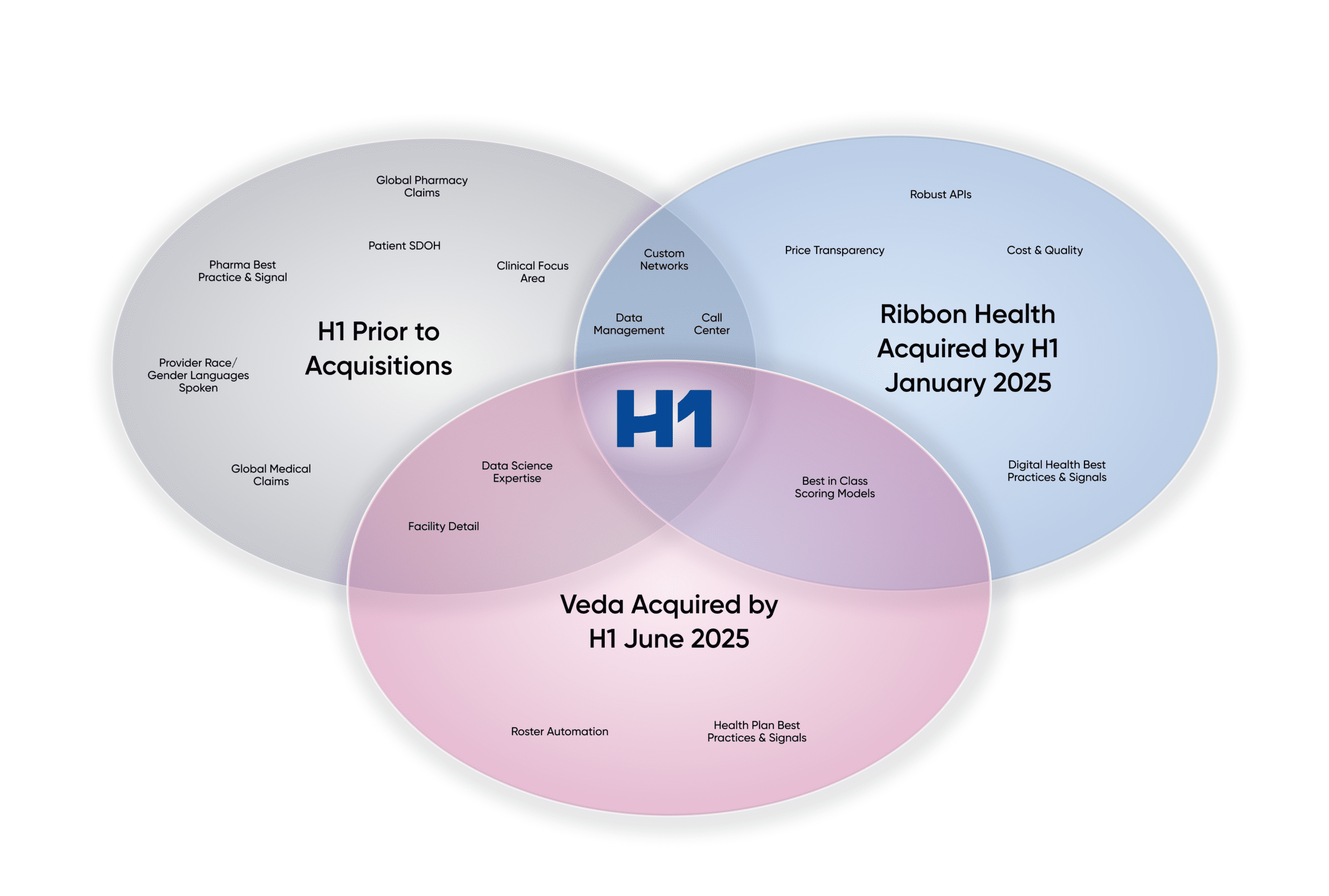
Together, we merge workflow efficiency, network precision, and the most in-depth real‑time accuracy into one integrated solution for health plans. The combined H1, Veda, and Ribbon solution gives you a modern provider data engine: automated, connected, and built to support accurate networks, compliant operations, and member experiences that keep people coming back.
What This Means for You
The combined solution is designed to address the core challenges plans face today: keeping data accurate, staying compliant, and delivering member experiences that build trust instead of frustration.
- Fewer errors, faster updates. H1’s combined platform is purpose-built to eliminate fragmented, outdated, and incomplete provider information that has historically plagued health plans.
- Operational lift. Automate what used to take weeks with continuous data refresh, while staying ahead of tightening regulations around directory accuracy.
- Data you can trust. Our AI‑powered confidence scoring gives you confidence in the accuracy of provider data, backed by integrated data accuracy models that continuously learn and improve over time.
- Better member experience. More accurate data creates smoother member experiences, higher satisfaction, and measurable retention gains.
The Confidence of Clarity
Together, the H1 platform gives you one provider data foundation built specifically for health plans. Now all H1 clients have the benefit of automated, connected, compliant data that works for network ops, compliance teams, and member experience.
