Provider Data Management
Create a single source of truth for your provider data
Transform disparate provider information into a unified, trustworthy database that fuels better member experiences by connecting them with the care they need.
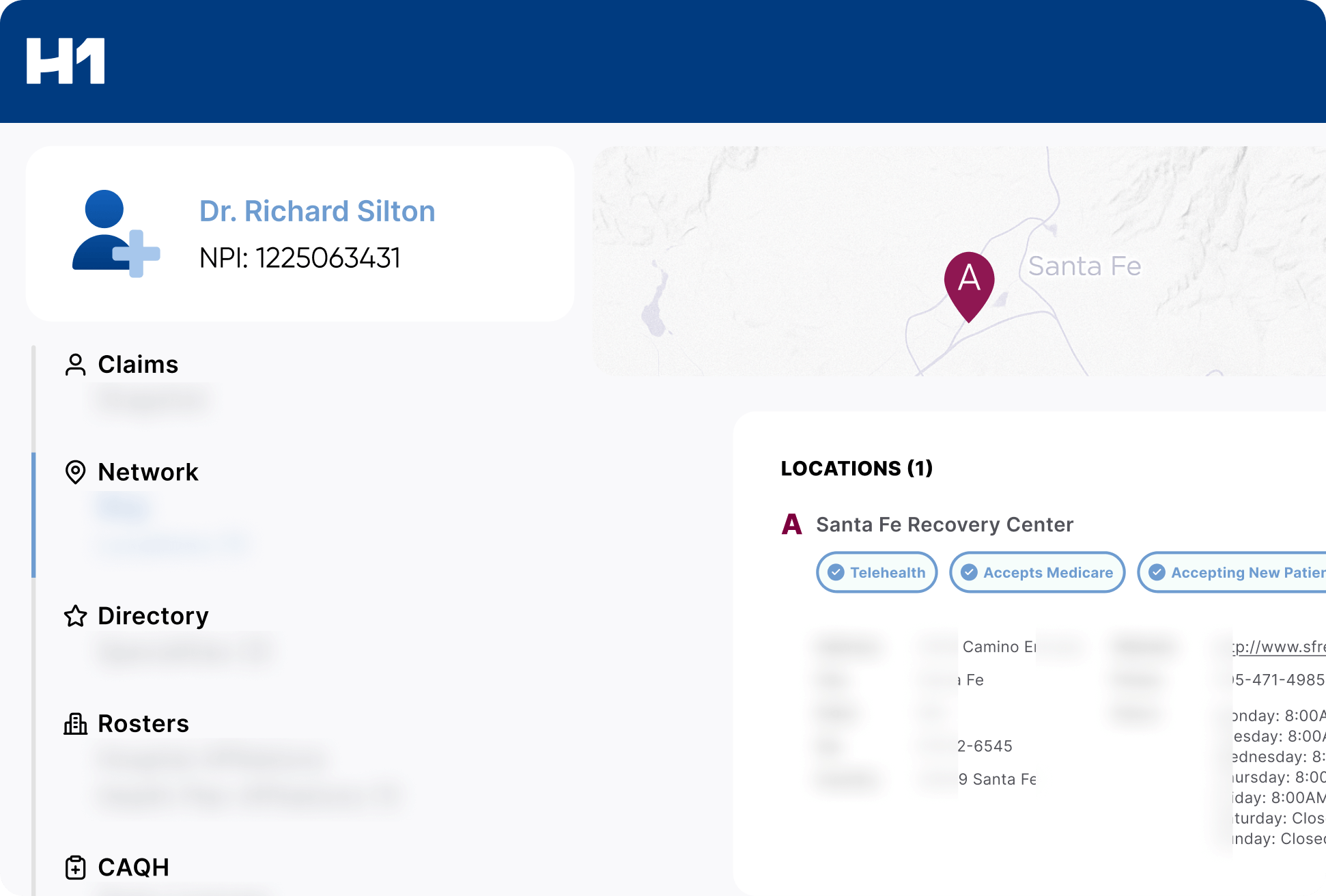
Build provider data excellence into every workflow
Provider data is scattered across systems, constantly changing, and notoriously difficult to maintain. H1’s Provider Data Management offers a complete solution to transform your data.
Single source of truth for all provider data
Powers accurate provider directories
Enables efficient claims processing
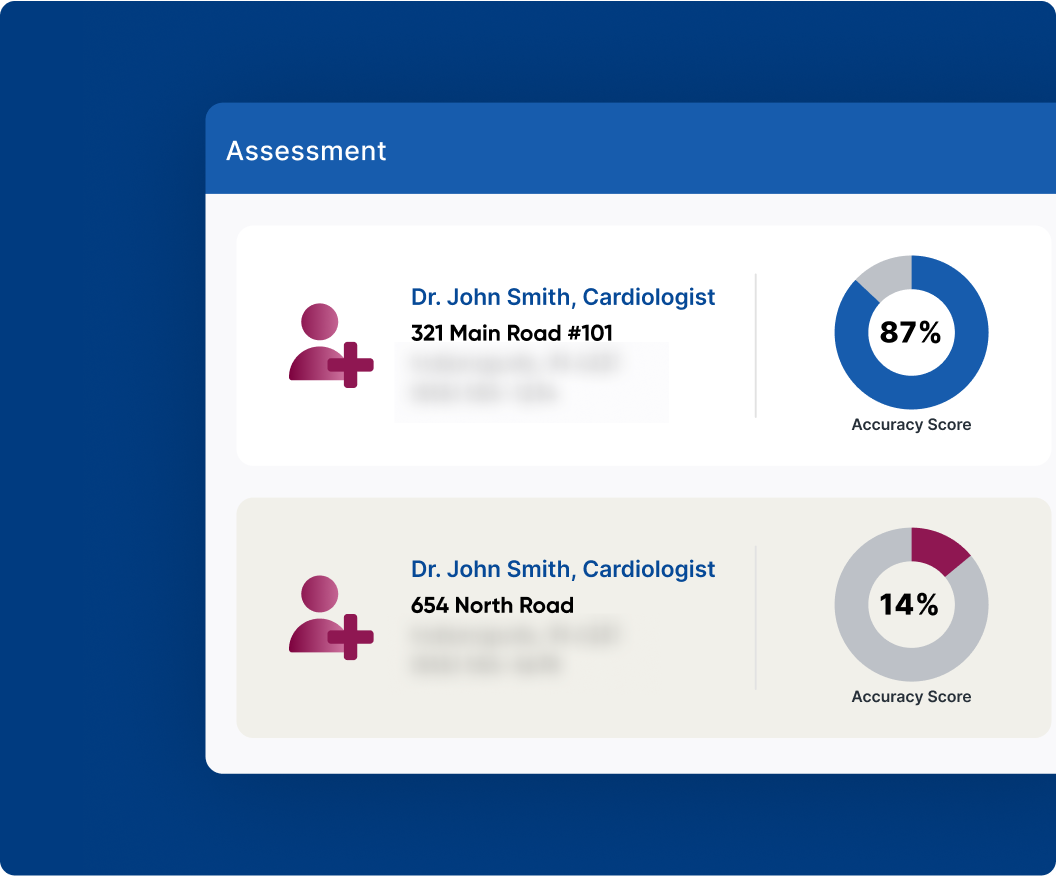
Ensure the best provider network
Eliminates data silos and inconsistencies
How it works
Transform provider data chaos by automating quality improvement at scale.
Provider Data Management that Delivers Results
$0.30
PMPM cost reduction for health plans
90%
accuracy across provider directories
55%
reduction in member complaints
5X
more productivity in data management

“H1 is the only end-to-end platform for managing provider data we’ve found. Their platform has significantly improved our overall accuracy and reduced our operating costs.”
VP, Provider Network Operations, Mid-Atlantic BCBS
Ready to revolutionize how data is managed?
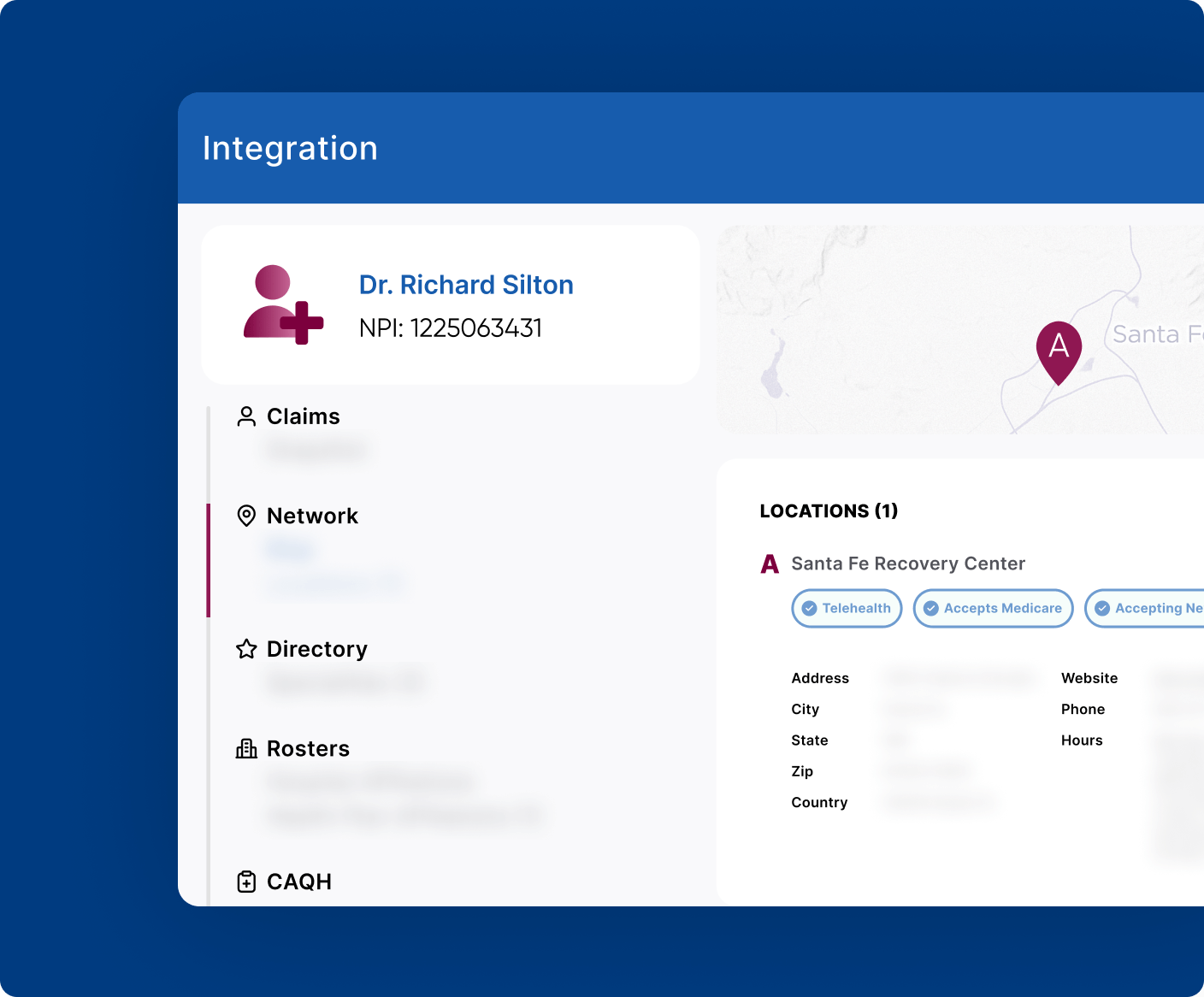
Implement custom business rules and logic tailored for seamless integration into your systems.